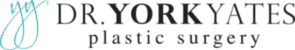Complications following breast augmentation may require revision. Revision breast augmentation surgery can be more complicated than the original operation. It is essential to choose a surgeon with skill and experience in breast augmentation to help avoid these complications. Should one arise, the surgeon must have the skill and expertise required to perform breast implant revision surgery. Click here to view our Breast Implant Guide.
Patients often research a breast augmentation revision more than they did for their original breast augmentation. They have a better understanding of how quality and experience of their plastic surgeon matters
Listed below are the major reasons patients choose breast implant revision, in order of how commonly we perform each operation.
Make sure to click the drop-downs for more information!
Changing Breast Implant Size
Choosing an implant size is an essential component of the breast augmentation consultation. In Dr. Yates’s office, the most valuable tools are “trying on” implants and 3D imaging. Occasionally, a patient will desire the exchange of implants for a larger or smaller size. A straightforward procedure with a very easy recovery.
Changing Saline to Silicone for Rippling
Silicone breast implants are softer and less likely to have rippling. Patients with saline implants who have issues with ripping or want a more natural feeling breast implant often change to silicone implants. A simple, relatively inexpensive procedure with little downtime.
Rippling occurs when the breast implant has a fold or ripple that is either seen or felt in the breast. All breast implants ripple to some degree, but most patients cannot feel or see this rippling as it is hidden by the breast and tissue covering the implant. Different implants ripple at different rates based on the amount and type of “fill” of the implant.
Rippling risk factors
- Thin patient with little coverage
- Saline implants
- Textured implants
- Implants with a lower fill ratio
- Implant material that is less cohesive (solid)
- Subglandular implants
Silicone implants tend to ripple less than saline as the fill material holds it shape better than saline. Of silicone implants, brands and styles of implants that are more cohesive tend to ripple less. Textured implants tend to ripple more than smooth because the implant shell is thicker.
For saline implants overfilling is a valuable tool to minimize rippling. This is commonly misunderstood to imply filling the implant more than it should be. The implant manufacturers have a fill range for saline implants, and overfilling is simply filling on the larger side of this range. Overfilling results in more firmness and roundness of the implant but is generally an acceptable trade-off.
Breast Implant Symmetry or Malposition Correction
Implant asymmetry and malposition are common problems requiring breast implant revision surgery. During breast augmentation, implant pockets are created and assessed for size and symmetry before implant placement. If the pockets are improperly formed, there will be breast implant asymmetry. Even well-designed implant pockets can have asymmetric settling of implant position from external effects such as muscle effects.
Treatment often requires modification of the implant pocket on one or both sides. This most commonly involves capsule tightening and muscle release procedures. The implant pocket modification is usually easy on the patient but tough on the surgeon. Easy on the patient because there is very little pain afterward, and the recovery is often much more comfortable than the original augmentation. Tough on the surgeon because symmetry is much harder to achieve than during the initial surgery.
Sometimes accurate repair will require more aggressive techniques. Sometimes changing the implant position relative to the muscle is necessary. Changing from above the muscle to below or vice-versa. If soft tissue is compromised and will not “hold” the implant into the desired position, additional support with synthetic or biological material can be added to support the implant. This is the so-called “internal bra” procedure. These materials aren’t without cost or complications, and Dr. Yates uses these as an added level of security or when other methods would not be expected to work.
Breast implant asymmetry issues
- Implant position asymmetry
- Pectoral muscle asymmetry (natural or caused from surgery)
- Capsular contracture
- Droop of the breast over implants
- Poor soft tissue support
The procedures used for improving breast asymmetry. Often in combination
- Keep implants in the same pocket and modify the pocket position
- Change from submuscular to subglandular or subfascial
- Change from subglandular to submuscular or subfascial
- Capsulectomy
- Additional of biological or synthetic support (Galaflex or Strattice for example)
- Breast lift
- Change of implant type
A plastic surgeon with vast experience in breast augmentation revision surgery can accurately diagnose the problems and have the knowledge base and experience required to fix the problem using a combination of the available tools.
Capsular Contracture Surgery
Capsular contracture is the development of an inappropriate amount of inflammation and scar tissue around a breast implant. It can cause unsightly or uncomfortable firmness of the breast. There are several suspected causes of capsular contracture. Two of the most commonly suspected reasons for increased inflammation and scarring around an implant are bacteria or blood.
To decrease the risks of capsular contracture, care and attention should be given to sterility during breast augmentation. Antibiotics are given before and after surgery, and the implants are “bathed” in antibiotic solution before implantation. Steps to decrease risks of bleeding at the time of surgery and afterward are also taken.
Factors that affect capsular contracture risk.
- Inframammary (breast crease) incision has the lowest risk as it avoids hidden bacteria in milk ducts
- textured implants have a lower capsular contracture rate than smooth implants
- submuscular pocket has a lower capsular contracture rate than subglandular
- #1 risk is the surgeon doing the surgery.Some surgeons, like Dr. Yates, have a <1% capsular contracture rate. Others can have rates as high as 20%. The reasons are multifactorial.
Early Capsular Contracture
Treatment of capsular contracture depends on the severity and how early it is diagnosed. If caught early, oral medications, including Vitamin E, antibiotics and Singulair, can be helpful. Massage, or even better, Acoustic sound wave treatment of capsular contracture, such as the Zimmer in Dr. Yates’s office, can be beneficial as well when caught early.
Late Capsular Contracture
The later presentation generally requires the removal of the implant capsule (total capsulectomy). The risks of recurrence can be reduced by changing to a pocket beneath the muscle if not already performed.
Replacing with Newer Implants
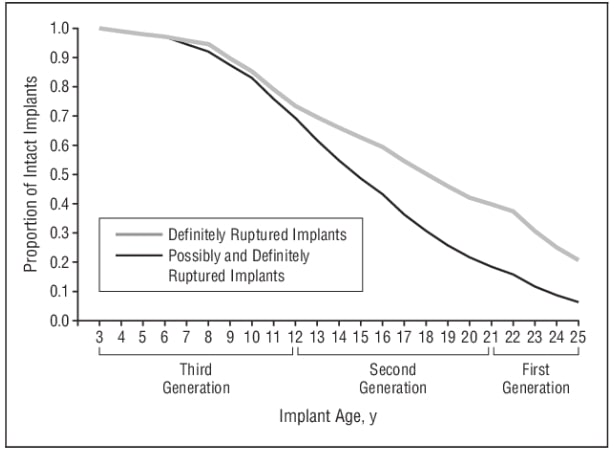
Breast implants are not intended to be lifetime devices. Breast implants rupture at a rate of approximately 0.5-1% per year for the first decade. The rupture rate becomes higher as time goes. Dr. Yates recommends replacement surgery in the 10-15 year range. And insists that all patients remove and replace with new implants by 20 years.
This is true of saline and silicone implants. There is some peace of mind with saline implants because “silent ruptures” are not possible. If saline implant rupture they simply go flat.
There is some evidence that our current generations of silicone implants, 4th and 5th are performing better than previous silicone implants shown on this curve.
Other reasons a woman may choose new implants are to change something cosmetically about their breasts. Examples are changes in implant sizes or types.
It is important for women to understand that just because the implant is “new” it doesn’t necessarily make the breasts look more youthful. Breasts age and the droop over an implant would not be expected to correct with a new implant. A breast lift or implant repositioning may be the procedure of choice.
Saline Breast Implant Deflation
Saline breast implant deflation requires removal of the deflated implant and replacement with a new implant. Generally, a straightforward procedure. The new implant position can be modified as necessary. The type and size of the implant can be changed as well. If the implants are older than 10 years we would recommend changing both sides. Breast implant manufacturers have warranties that may provide patients new implants free of charge.

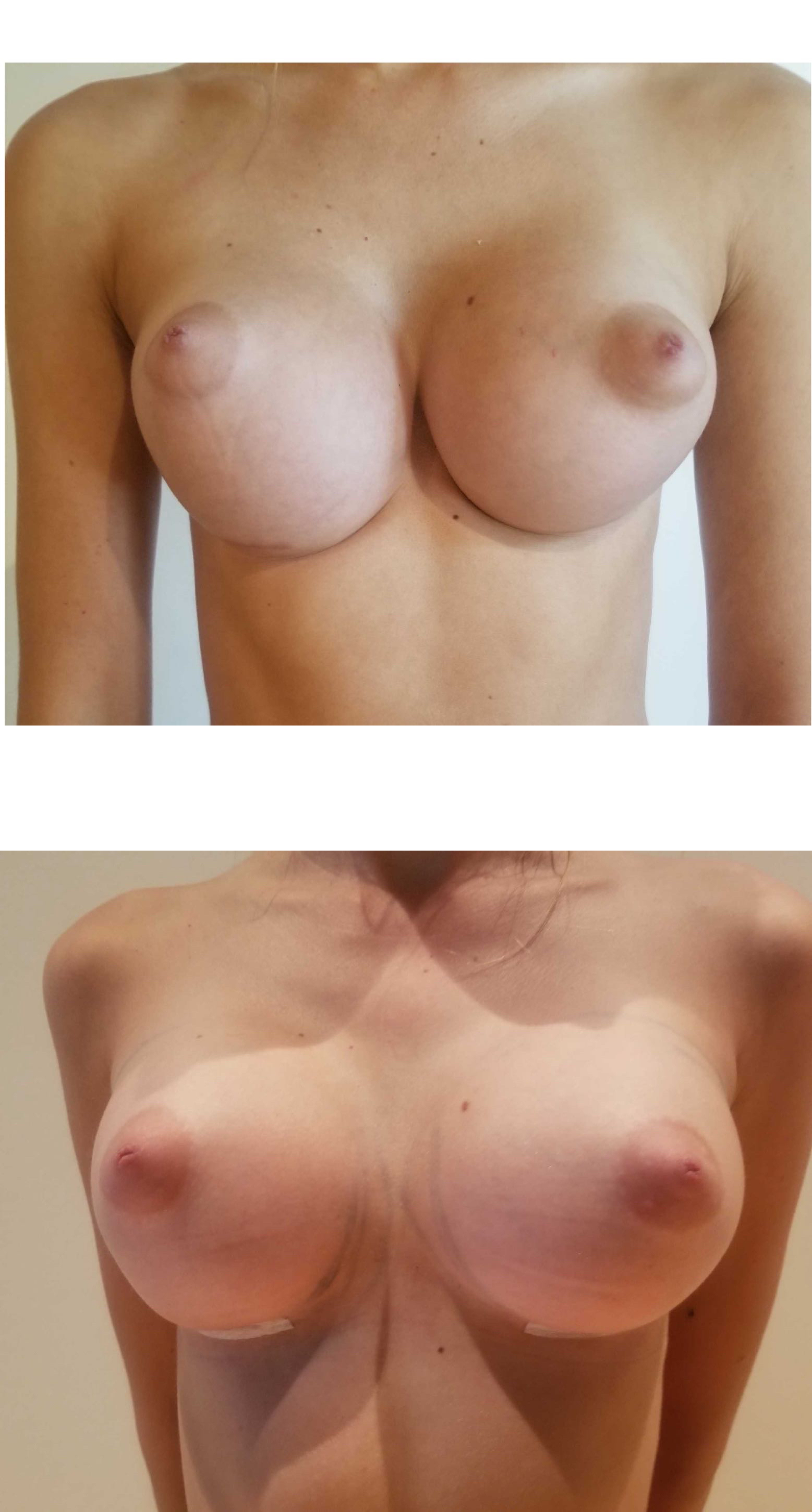
Silicone Breast Implant Rupture
Silicone implant rupture happens at a lower rate than saline implants but when it occurs, it is a more difficult problem. Silicone implant rupture generally requires removal of the silicone breast implant and all breast implant material. Occasionally, the capsule around the implant also requires removal. With newer generation cohesive silicone breast implants, the silicone is undoubtedly less “messy.” Watch the video of a case where I encountered a “silent rupture” of a silicone implant. The implant after removal is shown below.
Breast Implant Health Concerns (Breast Implant Illness)
“I believe my silicone breast implants are causing me to be sick, and I want them removed.”
This has been a concern of some patients for many years, but in light of social media, there has been renewed vigor of these concerns recently. Defenders of silicone implants will say that the data and science are conclusive. Silicone implants were taken off the market for over a decade, while rigorous testing and studies supported their safety. Proponents of breast implant illness claim that these studies were poorly designed and inconclusive.
Here is my (Dr. Yates) editorial and current belief on the issue… I don’t know. Sorry for the obscurity, but as a surgeon who has been placing, replacing, and removing silicone implants for years, I cannot say that I have definitively seen a patient with BII. I have had several patients that I have removed implants for presumed BII, and some of them report improved symptoms. But few of these symptoms are objective and measurable.
I believe Breast Implant Illness likely exists. Our bodies and our immune systems are so different; it would be unwise to deny that a rare population of people may react differently to any foreign body, including breast implants. My advice is that a patient considering breast augmentation should consider breast implant illness as well as a number of many other, more frequent, risks when making this decision. My advice to women who have implants and believe they may be causing illness is to see their Plastic Surgeon discuss these issues as well as their general medical doctor to rule out other conditions. Implant removal +/- capsule removal may be indicated. Click the link for my most recent blog post about breast implant illness.
Recalled Breast Implants
There is a relatively new disease process associated with breast implants called BIA-ALCL (Breast Implant-Associated – Anaplastic Large Cell Lymphoma). It is a cancer of the lymphatic system that has been associated specifically with textured breast implants. There is a much higher risk of ALCL with a specific type of breast implant texture called Macrotexture, made by Allergan. As of July 2019, these textured Allergan implants have been removed from the market. Although the FDA is not recommending implant removal or exchange unless symptoms develop, many patients who have these implants are having them removed and exchanged with smooth implants out of caution. As of Jully 2019, Allergan created the BIO CELL Replacement Warranty in which they will provide smooth-walled implants free of charge to replace textured Allergan implants.

Breast Implant Removal
Reasons for breast implant removal
- unhappy with size
- pain related to breast implants
- desire more natural breast shape
- recurrent problems such as capsular contracture or seroma
- poor cosmetic outcome
- health concerns related to implants
The cosmetic results of breast implant removal can range from fantastic to unacceptable. Factors including the size and location of breast implants, subsequent changes to the breasts after augmentation, and time the implants have been in place all affect the cosmetic outcome. Whether to remove the capsule around the implant is a matter of great debate. In Dr. Yates’s opinion there is little reason to remove a healthy capsule but the same is not true of problematic capsules. After removal, there may be cosmetic options to improve breast size, fullness, and shape such as a breast lift and fat transfer to the breast for patients who need them.
Seroma
Seroma is swelling of one breast. This can happen overnight or slowly. Most cases of seroma are related to textured implant. BIA-ALCL has to be considered and often worked up whenever a patient presents with a late breast seroma.
Breast Pain
Breast pain after breast implants can be related to the implant or breast tissue itself. In most cases, healing or irritated nerve endings are responsible. Revision surgery to improve breast pain is unpredictable as sometimes a cause for the pain can not be determined. Common treatable causes of breast pain after breast implants are capsular contracture, seroma, implant malposition, and implant folding or rippling.
Synmastia/ Symmastia
Synmastia is a loss of cleavage between the implants. It is also referred to as “breadloafing” or “uniboob” This results from a pocket created too far medially with the over-aggressive release of the implants medially. There is a higher risk when the implant is too large for the patients’ frame. Correction is complicated involving the re-creation of the medial pocket allowing the implants to separate, possibly supporting the tissue with acellular dermal matrix or synthetic support.
What type of anesthesia is used for Breast Revision surgery?

What about an Internal Bra with Breast Revision?
An internal bra procedure or an internal lift procedure can be a component of a breast revision surgery. With an internal bra procedure, a flexible, but strong, material is added to a breast lift or implant repositioning surgery to provide better support. Although there have been many materials utilized in the past few years, the most commonly used support material are Galaflex and Strattice. The material can be used inside the implant capsule to provide internal support or closer to the level of the skin for soft tissue support. There is additional cost and risk associated with using these materials and Dr. Yates doesn’t recommend it for routine cases. Rather, cases where soft tissue or capsule support would be expected to be problematic. Click the link to learn more about the “internal bra“.
How do I get a consult with Dr. Yates?
We would be honored to have you as our next breast augmentation patient. To schedule a consultation, call the office at 385.526.5988 or if you would prefer an online visit fill out a virtual consultation form. Dr. Yates will respond in a timely fashion to your inquiry.
Schedule a Consultation
Call us at 385.526.5988 to learn more about breast implants in Layton, UT, or schedule a consultation by contacting us here.