What is an Internal Bra?
The term “internal bra” can be used to describe a number of modifications in breast surgery but today, the term “internal bra” is most commonly used to describe the addition of soft tissue support to breast augmentation surgery. A key indicator of successful breast augmentation surgery is when implants heal in their intended position. Complications of implant position are not terribly uncommon, and implants can fail to drop appropriately or drop below their intended position, which is referred to as bottoming out. An internal bra is the addition of supportive material that acts as an insurance policy against bottoming out.

Should every Breast Augmentation patient receive an Internal Bra?
The answer to this question depends on the skill and experience of the breast augmentation surgeon doing the procedure. Dr. Yates has been doing breast augmentation for nearly two decades, and most of this experience was before the internal bra concept. Experience has taught Dr. Yates patterns of patients who are most at risk of bottoming out. Although it would be easy to simply recommend an internal bra to every breast augmentation patient, Dr. Yates finds that overwhelmingly most patients do not need an internal bra. The internal bra adds a significant expense and has the potential for complications much worse than the bottoming out it is trying to prevent, so using them on everyone is overkill at best.
Which patients benefit most from an Internal Bra?
Whereas the average breast augmentation patient does not benefit from an internal bra, there are situations where it may be helpful. Dr. Yates considers an internal bra a reasonable tool only in cases where there are factors that make a patient prone to implant bottoming out. Dr. Yates most often uses an internal bra in revision cases where patients have had difficult times with implant positions. It should be noted that most of these revisions are on other surgeons’ work, and we will often do revision cases without internal bras as well.
Here are a few of the patients where Dr. Yates may find benefit in an internal bra. This is not intended to be a complete guide, and patients would be wise to lean on the experience of their surgeon when making decisions such as these.
- Poor soft tissue support
- Very large and heavy implants
- Implant position above the muscle
- Patients who require release of their inframammary fold
- Revision cases where an implant has already bottomed out
- Revision cases with synmastia
- Revision cases where the implants have pushed laterally
- Revision cases with severe rippling where additional coverage is helpful
- Surgeons preference, such as surgeons who struggle with bottoming out
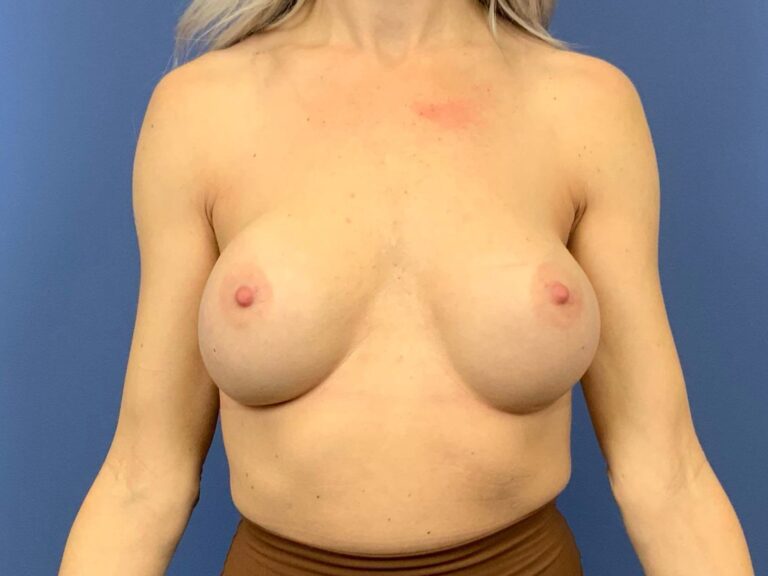
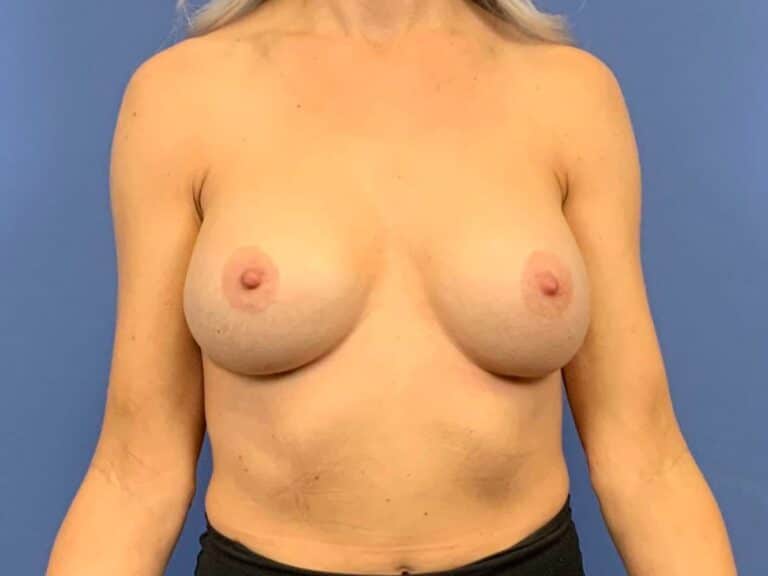
Why not use an Internal Bra for every Breast Augmentation patient?
Although there are potential benefits to using an internal bra, there are also drawbacks. First, there can be complications with the material itself; sometimes, they are much worse than the bottoming out they are trying to prevent. Complications such as:
- Mesh exposure requiring removal
- Infection
- Fluid build-up (seroma)
- Implant pocket deformity from mesh rippling or folding
- Implants that don’t settle the breast tissue droops over the implant (waterfall deformity)
- Poor expansion of the lower pole of the breast for some patients
Second, the internal bra is relatively expensive, increasing operating time and costs. There are good plastic surgeons who prefer to use an internal bra for many, if not most, of their breast augmentation patients. The reader should understand that surgeons’ techniques vary, as do outcomes and common complications. For any surgeon who finds that bottoming out is a common outcome adding an internal bra may be a good solution.
There are times when the patient has very poor inframammary support or when a patient chooses a very heavy implant Dr. Yates may recommend an internal bra for improved security and support.
Do patients in need of a Breast Lift need Internal Bras?
The internal bra is intended to support a breast implant, not necessarily the overlying breast tissue. If a surgeon determines a patient has a unique situation where the implant support would be expected to be compromised, or in revision cases where an implant has bottomed out, Galaflex/ Galaform may be indicated as an internal bra. However, there are breast lift cases where an internal bra could be counterproductive over time.
Here is an example; several years ago, textured implants were all the rage. The textured implants were designed to keep the implant in position, and they did a pretty good job of that. With this additional implant support, we saw more and more cases of breasts drooping over the implant. Particularly for women with heavy breasts without good natural skin support for their breast weight. The texture on the implant ONLY supported the implant, not the overlying soft tissue. A similar situation exists for an internal bra that supports the implant but could allow the overlying breasts to droop over the implant.
What is the best supportive material to create an Internal Bra?
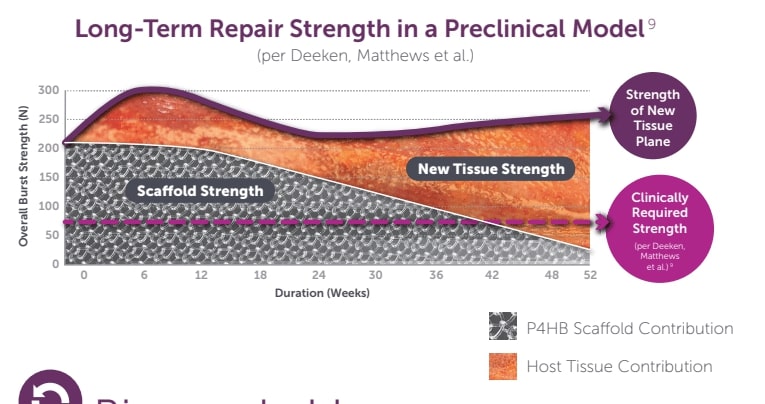
There have been dozens of materials developed with the intent of adding soft tissue support. Over the years, Dr. Yates has used many of these materials for both cosmetic and reconstructive indications. The gold standard for soft tissue support is ADM (acellular dermal matrix) which has been made from either human or pigskin. Dr. Yates now prefers Galatea (Galaflex) or Durasorb for most cases that require additional soft tissue support. Galaflex is made of poly-4-hydroxybutyrate (P4HB). This material has many benefits to previous generations of surgical scaffolds.
- Strength – 3-4 x as strong as native tissue
- It is entirely absorbed over time, leaving only supportive scar tissue.
- Naturally broken down to CO2 and H2O by 18-24 months
- Resistant to infection and seroma compared to previous materials
One disadvantage of Galaflex is that, in some cases, it is palpable and disturbing to the patient and has a very slow resorption timeline. Galaflex lite is a good alternative using thinner and less palpable material. Another great alternative for patients for whom palpability is a concern is Durasorb. Durasorb comprises a mesh pattern of commonly used suture material, PDO. This has some advantages to Galaflex in that it is a little more flexible, less palpable, and has a quicker resorption time. Essentially all of the product is gone by one year and replaced by supportive scar tissue.
Good Luck on your Breast Augmentation Journey
The goal of this article is to hopefully inform the reader about surgical soft tissue support, specifically the internal bra. We have had an increasing number of patients asking about this relatively new concept in breast augmentation, and hopefully, this helps patients understand both the advantages and disadvantages therein. This is an ever-evolving concept, and Dr. Yates will update this material as new information comes available.