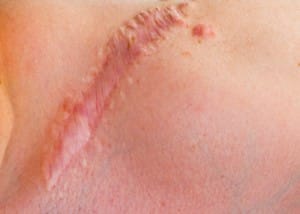
Surgical scars are the necessary, trade-off of many plastic surgeries. Many of these scars heal as only a faint white line. Some scars are unsightly, raised or even tender. There are four major factors that contribute to how a scar will heal:
- Surgical technique – Tension and alignment of the scar are important. Dr. Yates pays a great deal of attention to precisely close the incisions in a manner to help them heal with the best scar possible
- Genetics – Some people create great scars and some people heal with poor scars. Generally, elderly patients heal with good scars. Generally, individuals with darker skin and younger people heal with less favorable scars
- Location of surgery – some areas on the body are prone to poor scarring such as the sternal area, shoulders, and back. Areas with tension or motion such as the knees generally heal with poor scars. Facial scars often heal well.
- Aftercare – Limiting excess trauma and stretch to the scar in the first 6 weeks is important. Immature scars are at risk of widening or excess scar build up. Scar cream is helpful to hydrate and protect scars. The benefit of even the best scar creams is minor.
Of these, only the surgical technique and post-operative care are controllable. Many patients swear by a certain cream or ointment for scarring because their previous surgical scars faded. In reality, scars generally fade over the first year after surgery no matter what you do. Post-operative care of scars includes the prevention of bad scars and the treatment of bad scars. Scars can often be improved, complete scar removal is unfortunately not possible.
Early Treatment to Help Prevent Bad Scars
- Limit motion/ tension on the scar – This is particularly valuable in the first 6 weeks. Common locations of tension include the knees and back. Solid surgical technique requires placing long-lasting deep sutures on areas of tension such as a tummy tuck or breast lift with implants.
- Avoid sun/ UV rays – This tends to pigment maturing scars. Protect with SPF 15 or higher for at least 1 year after surgery
- Antibiotic ointment – (Neosporin, Bacitracin, Triple antibiotic ointment) – For open wounds only. Unnecessary for closed incisions. Studies have shown that moist wound healing is quicker and results in better scars. Antibiotic ointment helps to hydrate the wound with the added benefit of decreasing bacteria in dirty wounds.
- Scar creams
- Biocorneum -A topical silicone gel, only available in doctors offices. Typically $50-$100. We provide this free of charge to our patients. A small amount is applied to the scar twice a day for approximately 2 months.
- Mederma- A topical gel that is rubbed into the scar. The active ingredient is onion extract (alium cepa). Mederma is easy to use and easy to find in stores, costing $25 to $30.
- Scarguard – A topical silicone gel similar to Biocorneum. Available online for $30 a tube
- Biodermis Xeragel – Silicone ointment. Available online for $20 a tube.
- Adhesive tape – Dr. Yates will often place hypoallergenic paper tape on an early incision for a few weeks, particularly after a tummy tuck or breast surgery. Minimizing trauma, scar hydration and possibly pressure may account for this effectiveness
- Vitamin E – Topical Vitamin E is used extensively in scar therapy. There is little to no evidence that it improves scars.
- Silicone sheeting – see below. Early application of silicone sheeting in the first 2-3 months after surgery has been shown to decrease the risk of hypertrophic scarring. Particularly helpful for patients prone to hypertrophic scarring.
Treatment of Bad Scars After They Have Formed
- Silicone dressings – Silicone gel sheeting has been shown to improve scar appearance and symptoms. The mechanism is thought to be related to scar hydration, pressure, and ionic charge of the silicone. These are available at drug stores and online and are relatively expensive. Generally, the sheets are self-adhering and placed on the problematic scar for 23 hours a day.Each sheet can be reused several times. There are several options including sheets and ointments:
- Epiderm by Biodermis – Several options for shapes and sizes (perfect for breast surgery and tummy tuck surgery) ranging from $14 to $97 per sheet. Dr. Yates current preference.
- Circa-Care – about $50 for a 6″x6″ square, can be cut and reused for about a month.
- Xeragel by Biodermis – 100% silicone gel ointment for areas where silicone gel sheeting would be difficult
- Scarguard – Topical “brush on” application. In addition to silicone – has cortisone, and Vitamin E. Available in most drugstores for $25 to $65.
Treatment of Stretch Marks
Stretch marks are a unique type of scar in the dermis. Click here for a discussion about stretch mark treatment.
Dr. Yates scar treatment recommendations can be summarized as follows:
- Use sunscreen.
- Apply neosporin for the first two days if the wound is uncovered.
- If surgical tape is applied, keep it on for three weeks.
- Apply scar cream – Biocorneum, Mederma or Scarguard once the dressings have been removed.
- If the scar is red or pink but otherwise flat, be patient.
- If the scar begins to become raised, see Dr. Yates to initiate silicone gel sheeting therapy.
- In the patient known to be at high risk of hypertrophic scarring silicone sheeting can be used instead of scar cream for the first 2-3 months.